Important Questions
Click on a question below to find the answer. For other questions, contact our Customer Service department at 800-654-9728.
Top FAQs
I just had a baby. Do I need to add my newborn to my plan?
If you are a Priority Partners member, you must call Priority Partners Member Services at 800-654-9728 to report the birth. Once the delivery is reported, the Priority Partners Newborn Coordinator will help get your baby’s coverage added.
If you are not a Priority Partners member, please check with your health plan or the Maryland Department of Health.
My benefits have ended. How do I renew them?
Here’s how you can renew your health benefits:
- Online at Maryland Health Connection – Login to your account, then go to “Start New Application” from the Quick Links on the Account Home page
- Use the Maryland Health Connection mobile app
- Call the Maryland Health Connection Call Center at 855-642-8572 (TTY: 855-642-8573)
- In person at your local health department; or local Department of Social Services.
How do I enroll in a Managed Care Organization (MCO)?
You can enroll in an MCO and choose a primary care provider (PCP) through the Maryland Health Connection. You have three ways to apply:
- Online at marylandhealthconnection.gov
- With the Maryland Health Connection mobile app
- Call 855-642-8572 (TTY: 855-642-8573)
You will be able to choose your MCO as one of the steps in the process.
How do I get a new member ID card?
Log into your member portal, by clicking “Member Login” at the top of our website. You can also call Priority Partners at 800-654-9728.
How do I change my doctor?
You can change your primary care doctor (PCP) by logging into your member portal. You can also call Priority Partners at 800-654-9728.
For New Members
When do I call Priority Partners Customer Service?
Call Priority Partners any time you have a question or need help with your health care. To add a newborn or verify eligibility, you must call. Members can also use HealthLINK@Hopkins to get a member ID card, request a change to their primary care doctor (PCP), or update their address.
What is HealthLINK@Hopkins?
HealthLINK@Hopkins is your member portal. In HealthLINK, you can: view your benefits, check claims and referral status, send secure messages to and receive them from Customer Service, request a new ID card, search for a doctor, and select a new primary care doctor (PCP).
How do I register for an account?
Click “Member Login” at the top of ppmco.org. Select “Member Register” under First Time Logging In? on the right side of the page. On the next page, enter your member ID, name, birthdate and gender. Then follow the steps to create a user ID and password. Your password must be nine characters and must contain at least one uppercase letter, one lowercase letter, one number, and one special character, such as #, * or @. Usernames and passwords are case-sensitive.
Remember: Your password is private. Do not write it down or keep it in a public space. Once the process is complete, you will be able to access your account.
Now that I’m logged in, how do I get started?
Once you’re logged in, you will see a welcome message on your homepage. This message will change to keep you up-to-date and informed on health issues. Start browsing the site by using the links located in the top navigation bar. They are organized by different sections including My Providers, My Health Plan, My Resources and My Preferences. You will also find a list of Quick Links in the left column of tasks most used by Priority Partners members.
How do I get a new member ID card?
Log into your member portal, by clicking “Member Login” at the top of our website. You can also call Priority Partners at 800-654-9728.
What doctors can I see as a Priority Partners member?
Go to the Find a Doctor section of this website or call Priority Partners at 800-654-9728.
Plan Coverage
When do I call Priority Partners Customer Service?
Call Priority Partners any time you have a question or need help with your health care. To add a newborn or verify eligibility, you must call. Members can also use HealthLINK@Hopkins to get a member ID card, request a change to their primary care doctor (PCP), or update their address.
If I pay the full price for a prescription, will Priority Partners reimburse me?
Yes, as long as the prescription is on the list of medications covered by Priority Partners. Within two weeks of purchase of the prescription, you may be eligible for reimbursement at the retail pharmacy. You may also submit your prescription receipts for reimbursement within 180 days of the date of service. For additional information, call Priority Partners Customer Service at 800-654-9728.
How do I find out more information about medication prior authorization?
Some medications require prior authorization from your plan before they can be dispensed by your pharmacy. This helps us ensure that your prescriptions are medically necessary. To determine if a medication requires prior authorization, look at the Pharmacy Formulary. Medications that require prior authorization are listed in the formulary as “PA.”. Your doctor can request these medications by submitting a prior authorization request. Information about covered medications, medication prior authorization requirements and pharmacy plan benefits are available here.
What is a Referral?
A referral is a written order from your primary care doctor (PCP) giving you permission to see a specialist or receive certain medical services. Before you can see a specialist and be covered for that care, you will need a referral from your PCP. For information on getting a referral for care, refer to your Priority Partners Member Handbook.
What is a Prior Authorization?
Certain medical services and supplies require approval before they will be covered by your plan. Prior authorization, also called prior approval or preauthorization, is the process where a qualified health care professional reviews and determines if a service is medically necessary. Your Summary of Benefits indicates which services, supplies or medications require prior authorization. All prior authorization requests are coordinated through your doctor’s office. Your doctor must ask for and receive approval before you receive certain care. Priority Partners will review the service, drug or equipment for medical necessity. If prior authorization is not given, then coverage for care, services or supplies may be limited or denied. Any costs for denied services that were the result of an in-network provider failing to receive prior authorization are not your responsibility. For more information on prior authorization guidelines through your Priority Partners plan, refer to your Priority Partners Member Handbook.
How long does it take for my benefits to start?
The Maryland Department of Health strives to process applications within days of receiving them. Once your application is approved, you have 28 days to select one of the HealthChoice MCOs to provide your health benefits. Services become available 10 days after you choose an MCO.
I just had a baby. Do I need to add my newborn to my plan?
If you are a Priority Partners member, you must call Priority Partners Member Services at 800-654-9728 to report the birth. Once the delivery is reported, the Priority Partners Newborn Coordinator will help get your baby’s coverage added.
If you are not a Priority Partners member, please check with your health plan or the Maryland Department of Health.
My benefits have ended. How do I renew them?
Here’s how you can renew your health benefits:
- Online at Maryland Health Connection – Login to your account, then go to “Start New Application” from the Quick Links on the Account Home page
- Use the Maryland Health Connection mobile app
- Call the Maryland Health Connection Call Center at 855-642-8572 (TTY: 855-642-8573)
- In person at your local health department; or local Department of Social Services.
Can I see my child’s or spouse’s information if they are under my plan?
If you are a Priority Partners member, this feature is unavailable because all members have individual HealthLINK accounts. Call Priority Partners Customer Service at 800-654-9728 with questions.
Finding Care
How do I search for a provider?
Click “Search a Provider” in the left column under Quick Links or, under the My Health Plans tab in the top navigation bar.
What doctors can I see as a Priority Partners member?
Go to the Find a Doctor section of this website or call Priority Partners at 800-654-9728.
Do I need to contact Priority Partners before going to the emergency room?
No. For life-threatening emergencies, call 911 or go the emergency room. After, call your primary care doctor within 24 hours to let him or her know about the emergency. However, if you have a problem after normal business hours that is not a medical emergency, you can receive services at an urgent care center. Directions on how to find a center are provided in the “Where can I find an urgent care center?” question below.
Who or where do I call for eye/vision care?
Your vision care is through Superior Vision. Call Superior Vision at 800-428-8789 or go to their website.
Who or where do I call for dental care?
Dental care is provided by the Maryland Healthy Smiles Dental Program. Call 855-934-9812 or visit their member website for more information or to find a dentist.
How do I change my doctor?
You can change your primary care doctor (PCP) by logging into your member portal. You can also call Priority Partners at 800-654-9728.
Why aren’t there any results when I search for a provider?
First, make sure you are spelling the provider’s name correctly. If you are not sure of the spelling, type in the first three letters and a list of all doctors with a last name starting with those letters will be displayed. You can then browse the list manually. Your search may also be too narrow, meaning there are no providers with your selected criteria within your network. Broaden your search by typing “%%” in a field or leaving it blank. This will generate all providers within those fields. Your search may also be too broad, meaning there are far too many providers with your criteria for a list to be generated. You can narrow your search by selecting an option in a field. A list will find and display only those doctors that fit your criteria.
What is a Site of Service?
Site of service is a term used to indicate the facility in which you receive care. Many surgical procedures can be performed safely in an outpatient hospital setting, such as an ambulatory surgery center (ASC). Certain procedures require prior authorization when performed in an outpatient hospital setting. For information on covered outpatient services, refer to your Priority Partners Member Handbook.
How do I find care for mental health or substance use disorder?
If you have a substance abuse or mental health question or concern, or want treatment options, please call Carelon Behavioral Health at 800-888-1965; (TTY 711).
Where can I find an urgent care center?
You can find an urgent care center near you in three easy steps.
- Go to the “Find a Doctor” and enter your ZIP code or select your state from the drop-down menu.
- Click the “Hospital or Facility” option, then click the “Search Providers” button.
- From the search results page, find the “Specialty” search category on the right side, and select “Urgent Care Center” from the drop-down menu.
Claims & Appeals
How do I file an Appeal?
Appeals must be submitted in writing 60 days from the date of the denial notice to the following address:
Priority Partners
Attention: Appeals Department
7231 Parkway Drive, Suite 100
Hanover, MD 21076 or Fax: 410-762-5304
Why aren’t my claims appearing?
Claims status takes 2 to 5 business days to update. If you’d like to confirm receipt or check the status of a claim, you can also call Customer Service at 800-654-9728.
Member Information
How can I order a new member ID card?
You can easily request a new ID card by logging into HealthLINK. Under My Health Plan, click Member Information then click on Request ID Card. Select the box next to your name and press Submit. The request will be automatically sent to your Customer Service department who will process the request.
You can also download the Request an ID Card form, fill it in and fax it to 410-424-4991. Or, you can call our Customer Service department toll-free at 800-654-9728.
How can I change my Primary Care Provider (PCP)?
Under Quick Links, click “Change Your PCP” or, under My Health Plans, click “Change PCP.” If you know the name or practice of the doctor you’d like to choose, type it in. You can search for a new PCP in your area by selecting from the drop down and typing the city, county or zip code in the field to the right. You can also search by the hospital the physician is affiliated with, by the sex of the doctor or by the language the physician speaks. Once you press Submit, browse through the list of doctors and press Select when you find the physician you would like. This request will go directly to your Customer Service department who will process the request. Approved change requests will take effect on the date the request is submitted. You will also get a new ID card mailed to you within 7 to 10 days of the approval.
How can I update my address?
Address changes must be made through the Maryland Health Connection and cannot be done through HealthLINK. Follow these directions to change your address.
- Log in to your account.
- Click on Report a Change under the Quick Links section on the right side of the page.
- Click Next.
- Select the Change Home Address checkbox as it applies to you.
- Click Next.
- If you have other changes to make to your account, check the boxes as they apply to you, then click Next. If you do not need to make any other changes, keep clicking Next until you reach the summary page.
- Click Confirm after reviewing your summary information.
- Answer questions about Special Enrollment.
- Review and Confirm all sections of application.
- Type your name in the Signature box exactly as it appears (or will appear) on your Maryland Health Connection account.
Maryland Health Connection phone number: 855-642-8572
Important: After you have updated your address in your Maryland Health Connection account, remember also to update your address with Priority Partners. Keeping your address information current with Priority Partners is necessary so you may continue to receive member services and important announcements or updates to your benefits.
Can I see my child’s or spouse’s information if they are under my plan?
If you are a Priority Partners member, this feature is unavailable because all members have individual HealthLINK accounts. Call Priority Partners Customer Service at 800-654-9728 with questions.
Medicare FAQs
What is Medicare?
- Medicare is health insurance from the federal government.
- It helps pay for doctor visits, hospital care, and medicine.
- Most people get Medicare when they turn 65.
- Some younger people with certain disabilities can also get it—like people with kidney failure or ALS.
- If you’re already getting Social Security, you’ll be signed up automatically.
How do I sign up?
- If you’re already getting Social Security, you’ll be signed up automatically.
- You need to sign up yourself if you’re not yet getting Social Security or Railroad benefits when you turn 65 (or earlier). People can sign up when they turn 65
- People can sign up when they turn 65
- 3 months before their birthday
- The month of their birthday
- Or 3 months after
Can I get help paying for Medicare?
- Yes. Help may be available:
- Extra Help for drug costs (If you have limited income and resources, you may qualify for Extra Help to pay for prescription drug costs)
- Medicare Savings Programs (This program can help pay for some of the costs associated with Medicare, such as premiums, deductibles, and co-pays. Eligibility is based on income and resources.) to help pay premiums and other costs.
- Programs like Qualified Medicare Beneficiary (QMB) (Helps pay for Medicare Part A and Part B premiums, deductibles, and co-pays. If you qualify for QMB, you will also automatically qualify for Extra Help with prescription drug costs).
- Specified Low-income Medicare Beneficiary (SLMB) based on income (Helps pay for Medicare Part B premiums).
- To apply or learn more about these programs, you can visit Maryland.gov.
What’s the difference between Medicare and Medicaid?
- Medicare is a federal program primarily for people 65 and older, or younger individuals with disabilities. It covers hospital, medical, and prescription drug services.
- Medicaid is a joint federal-state program that provides health coverage to low-income individuals, including children, pregnant women, and people with disabilities.
- Eligibility: Medicare is age- or disability-based, while Medicaid is income-based.
- Some people qualify for both – this is called “dual eligible” or a DSNP plan.
What if I have more questions?
Call our Customer Support team: 800-654-9728 (TTY: 711)
We can explain how Medicare works and help you understand your options.
Plan Perks
How do I claim my preventive care visit gift card?
Eligible Priority Partners members may receive a reward for having certain health care services. Visit ppmco.org/rewards to find out more or call Member Services at 844-288-9593.
HealthLINK Account
Why aren’t my claims appearing?
Claims status takes 2 to 5 business days to update. If you’d like to confirm receipt or check the status of a claim, you can also call Customer Service at 800-654-9728.
What is HealthLINK@Hopkins?
HealthLINK@Hopkins is your member portal. In HealthLINK, you can: view your benefits, check claims and referral status, send secure messages to and receive them from Customer Service, request a new ID card, search for a doctor, and select a new primary care doctor (PCP).
How do I register for an account?
Click “Member Login” at the top of ppmco.org. Select “Member Register” under First Time Logging In? on the right side of the page. On the next page, enter your member ID, name, birthdate and gender. Then follow the steps to create a user ID and password. Your password must be nine characters and must contain at least one uppercase letter, one lowercase letter, one number, and one special character, such as #, * or @. Usernames and passwords are case-sensitive.
Remember: Your password is private. Do not write it down or keep it in a public space. Once the process is complete, you will be able to access your account.
How do I set up two-factor authentication?
When you try to log into HealthLINK, after entering your user name and password, you will be brought to this page:
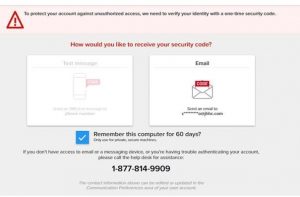
You will be prompted to receive a security code either through text, (if you have a cell phone number listed in your account) or by email. If you don’t have a cell phone number listed in your account, you can add it later by scrolling down to the ‟Communication Preference” section of the Administration tab. (see the NOTE for instructions). If you request the code through email, and it does not appear in your inbox, check the spam/junk folder.
Enter the security code on the next screen:
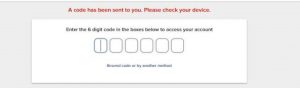
NOTE: Changing Communication Preferences
After completing the two-factor authentication process using your email and successfully entering the HealthLINK portal, go to the Administration tab and scroll down to Communication Preferences.
- Go to “Edit Contact Details”
- Enter your mobile number and click “Save.”
Now that I’m logged in, how do I get started?
Once you’re logged in, you will see a welcome message on your homepage. This message will change to keep you up-to-date and informed on health issues. Start browsing the site by using the links located in the top navigation bar. They are organized by different sections including My Providers, My Health Plan, My Resources and My Preferences. You will also find a list of Quick Links in the left column of tasks most used by Priority Partners members.
What happens if I can’t remember my password?
When registering for a HealthLINK@Hopkins account, you will be asked two security questions. If you ever forget your password, you can reset your password by giving your username. You will have 24 hours to click on the link sent to your email. When you click on the link, you will be asked to answer the security questions. If you enter the wrong password three times, your account will be locked and you will have to call the HealthLink help desk at 877-814-9909. The help desk will ask you your security questions. If you do not answer correctly, you will be locked out of your account until Priority Partners is notified and can verify your membership. You will be contacted upon verification and you will then be able to reset your password and access your HealthLINK account.
How do I search for a provider?
Click “Search a Provider” in the left column under Quick Links or, under the My Health Plans tab in the top navigation bar.
How can I order a new member ID card?
You can easily request a new ID card by logging into HealthLINK. Under My Health Plan, click Member Information then click on Request ID Card. Select the box next to your name and press Submit. The request will be automatically sent to your Customer Service department who will process the request.
You can also download the Request an ID Card form, fill it in and fax it to 410-424-4991. Or, you can call our Customer Service department toll-free at 800-654-9728.
How can I change my Primary Care Provider (PCP)?
Under Quick Links, click “Change Your PCP” or, under My Health Plans, click “Change PCP.” If you know the name or practice of the doctor you’d like to choose, type it in. You can search for a new PCP in your area by selecting from the drop down and typing the city, county or zip code in the field to the right. You can also search by the hospital the physician is affiliated with, by the sex of the doctor or by the language the physician speaks. Once you press Submit, browse through the list of doctors and press Select when you find the physician you would like. This request will go directly to your Customer Service department who will process the request. Approved change requests will take effect on the date the request is submitted. You will also get a new ID card mailed to you within 7 to 10 days of the approval.
How can I update my address?
Address changes must be made through the Maryland Health Connection and cannot be done through HealthLINK. Follow these directions to change your address.
- Log in to your account.
- Click on Report a Change under the Quick Links section on the right side of the page.
- Click Next.
- Select the Change Home Address checkbox as it applies to you.
- Click Next.
- If you have other changes to make to your account, check the boxes as they apply to you, then click Next. If you do not need to make any other changes, keep clicking Next until you reach the summary page.
- Click Confirm after reviewing your summary information.
- Answer questions about Special Enrollment.
- Review and Confirm all sections of application.
- Type your name in the Signature box exactly as it appears (or will appear) on your Maryland Health Connection account.
Maryland Health Connection phone number: 855-642-8572
Important: After you have updated your address in your Maryland Health Connection account, remember also to update your address with Priority Partners. Keeping your address information current with Priority Partners is necessary so you may continue to receive member services and important announcements or updates to your benefits.
What is a secure message and how do I send one?
A HealthLINK@Hopkins secure message is similar to an email. As a member, you are able to send messages to and receive them from the Customer Service department and your Care Manager (if you are assigned one). To get started, click on “Message Center” in the top-right corner of your screen. From there, click “New,” and a new message box will open. Click on the Directory link for a list of possible recipient mailboxes. Type the mailbox name of the person or department you would like to message in the Search For field. The number of unread messages in your inbox will appear next to the envelope symbol in the top-right corner. You can view your sent, deleted and inbox mail by clicking Message Center and selecting the appropriate gray tab.
The HealthLINK secure message portal is intended for use only by Priority Partners members. If you are an Advantage MD member in need of assistance, please do not use this portal. Contact Advantage MD Customer Service for help with your specific plan.
What is “View Audit”?
This button allows you to see all of your account transactions. If you would like further information about any of the transactions, write down the complete transaction ID and contact Customer Service. The Customer Service numbers can be found below, or you can send a secure message by clicking “Message Center” in the top-right corner of the HealthLINK@Hopkins screen.
Can I see my child’s or spouse’s information if they are under my plan?
If you are a Priority Partners member, this feature is unavailable because all members have individual HealthLINK accounts. Call Priority Partners Customer Service at 800-654-9728 with questions.
How do I get a new member ID card?
Log into your member portal, by clicking “Member Login” at the top of our website. You can also call Priority Partners at 800-654-9728.
Diabetes Supplies
Which blood glucose meters are covered?
ADC’s Freestyle® and Precision Xtra® blood glucose meters are covered. These meters are available to Priority Partners members at no cost.
How can I obtain a free meter?
Here are three ways for Priority Partners members to obtain a blood glucose meter at no cost:
- Call Abbott Diabetic Care (ADC) at 800-680-6850
- Order online at www.ChooseFreeStyle.com
- Visit your local pharmacy and request a free meter
If you have any questions, please call Priority Partners Customer Service at 800-654-9728
What information do pharmacies need to provide a no-cost ADC meter?
Your pharmacy can dispense a free meter without a prescription using the information below:
- RxBIN No.: 610020
- Group No.: 99992432
- ID No.: ERXPARTNER
Vaccine Information
What is a vaccine or immunization?
A vaccine is a type of medicine that is usually given to you as a shot with a needle. The medicine in the shot protects your body from one or more diseases. When you get this medicine, your body learns how to fight the disease so that you will not get sick from it. This is called “immunization.”
Why does my child need vaccinations?
Vaccines help the people who get them because they prevent them from getting diseases or infections that could make them sick or even kill them. They also help the vulnerable, unvaccinated people around them because it reduces the spreading of diseases and infection if most people are vaccinated and are not contracting them in the first place.
Are vaccines safe?
Yes. Vaccines are very safe. If any side effects occur from vaccinations, they are very minor, such as soreness where you received the shot, fussiness; or a low-grade fever. Serious side effects, like allergic reactions, are very rare, and doctors are trained to treat them.
My child doesn’t like shots. Is there another way to get vaccinated?
Some vaccines can be taken by mouth or sprayed into your nose. Talk to your doctor to see whether this is an option. Most of the time, you will need to have the shot with a needle. It may sting for a moment and be a little sore, but it is much better than taking the risk of getting sick. Putting a cool, wet wash cloth where you got your shot can help make it feel better.
Why do we get the same shot more than once?
Some vaccines take more than one dose to give you full protection. Other vaccines stop working after a while, so you need to get them again. Make sure that you get every dose of all of your vaccines. This is the only way to make sure that you are protected from the disease.
Why do vaccinations start so early?
Babies and young children need to be vaccinated because they are more at risk for diseases. These diseases can also be much more serious for infants and young children.
How do I know which vaccines my child needs?
Talk to your child’s doctor about what vaccines they need. You can also look at these charts that tell you what vaccines your child needs based on how old they are.
Where can I get a flu shot?
Priority Partners members can receive a flu shot at their primary doctor’s office or at one of many flu network pharmacies, including CVS, Walgreens, Walmart, Rite Aid, and more. Find a nearby pharmacy.
Can the flu shot give me the flu?
No, the flu shot cannot cause flu illness. The viruses contained in flu shots are inactivated (killed), which means they cannot cause infection.
How much does it cost?
You will not be reimbursed for flu vaccines paid out of pocket. Please make sure to go to one of our vaccine network flu pharmacies where your flu vaccine will be free!
Find a pharmacy in our vaccine network where you can get the flu vaccine.
Are there different types of flu shots?
There are different types of flu shots, and the CDC recommends you receive whatever is available at your pharmacy or doctor’s office.
Which brands of the flu vaccine are covered at network flu vaccine pharmacies?
All standard Trivalent and Quadrivalent available brands of the flu vaccine, including FluMist (nasal spray), are covered at network flu vaccine pharmacies.
Fluzone intradermal, sort needle vaccine, and the Fluzone High Dose formulations are not covered at the retail pharmacy.
If you have questions about the flu, read more about it at www.cdc.gov/flu.
What other vaccines can I get at the pharmacy instead of my PCP’s office?
Shingrix is a vaccine against the Herpes Zoster that can be administered by your doctor or your pharmacist at a vaccine network pharmacy. A prescription is needed when you obtain the vaccine from a pharmacy.
Adult pneumococcal vaccine, for pneumonia prevention, can be administered by your doctor or your pharmacist at a vaccine network pharmacy. A prescription is needed when you obtain the vaccine from a pharmacy.
Members may obtain vaccines from a network provider or the vaccines below from a network pharmacy. The list below identifies vaccines available at a vaccine network pharmacy at no cost.
| Vaccine | Use | Copay* | Recommended Age |
|---|---|---|---|
| Flu Vaccine | Flu prevention | $0 | Age 19 and over |
| Shingrix | Shingles prevention | $0 | Age 50 and over |
| Adult Pneumococcal | Pneumonia prevention | $0 | Age 19 and over |
*When administered at a Vaccine Network Pharmacy
Is there an age restriction for vaccines?
Your doctor can determine if you should receive a vaccine based on CDC recommended guidelines.
Asthma Medication
Does my child need to take their asthma medication?
Yes, your child needs to take their asthma medicine as long as their doctor tells them to. Do not stop taking the medicine without first talking to your child’s doctor. Your child may not have any asthma symptoms, but the medicine helps to keep it that way.
How do I remember to fill the prescription each month?
Talk to your pharmacy about getting reminders. Most pharmacies will send refill reminders to you by call, text, or email when it is time to get a refill.
How can I obtain a nebulizer?
Call Priority Partners at 800-654-9728.
How can I get a ride to my child’s doctor?
If you do not have a way to get to your child’s doctor, Priority Partners can help you get a ride. Please call 888-500-8786 for information.
How do I pay for it?
You do not need to pay for this medicine. It is covered through your child’s Priority Partners benefits. There is no copay for pregnant adults or children under the age of 21.
What else can I do to help my child breathe easier?
Avoid things that worsen your child’s asthma. Things that can make asthma worse are called triggers. Triggers can be dust, mold, animal fur and saliva, pollens and grasses, smoke, or perfumes. Your child should not avoid exercise. Exercise is important for your child’s health.
Are steroid inhalers safe?
Steroid inhalers are different than the muscle-building steroids sometimes abused by athletes. This medicine is breathed in, so it only goes to the lungs. There may be a slight slowing of growth for children by using a steroid inhaler, but this is rare. The benefit of your child breathing better is worth it for most parents.
I lost the prescription for my child’s asthma medication. What do I do?
Call your child’s doctor to get a new prescription. Sometimes, they can send the prescription to your pharmacy, or they may want to see your child in the office if they haven’t had a visit recently.
Is the asthma medication prescribed to my child safe?
Yes, asthma medicines are safe when given by your child’s doctor. Be sure to follow the directions from your doctor and pharmacist. Do not give your child extra medicine or inhaler puffs unless your child’s doctor tells you to.
Transportation
I do not have a way to get to my doctor’s office. What should I do?
Priority Partners can arrange free rides to and from doctor’s appointments for members, as long as they are for medical appointments and meet all qualifications.
What other transportation options do I have?
Members who need transportation services should first consider these questions:
- What have I done in the past to get to my medical appointments?
- Have I contacted my local health department to ask about transportation services?
- Is there someone in my household who can give me a ride?
- Do I have friends or family members outside of my household who can take me?
- What have you done to explore other options for transportation when it was needed?
Members who have explored these options and also meet the eligibility requirements can request transportation services through Priority Partners at 800-654-9728. Members may find additional transportation services help at 211md.org or findhelp.org.
Who is eligible for transportation services?
All Priority Partners members who meet the following requirements are eligible for transportation services:
- PPMCO will need to verify same-day urgent care visit with your primary care doctor.
- You need to see a specialist who is more than 30 miles away, and there is not a provider located closer to your home.
- You have been referred/approved for an eligible service or screening exam.
- Your local health department has denied you transportation services. We can help you find out why.
- You have a confirmed screening exam listed below:
- Your primary care doctor for a confirmed urgent same-day visit
- Primary care visit
- Prenatal exam
- Postpartum visits between 7 and 84 days after giving birth
- Adult or child SSI visits
- Child lead screening
- A1c screening
- Diabetic eye exam
- Diabetic Kidney Exam
If you need help scheduling one of the above appointments with transportation included, call Member Services at 800-654-9728 (TTY: 711).
What doctor visits are approved for transportation services?
Members can only use transportation services for these eligible medical appointments:
- Your primary care doctor for a confirmed urgent same-day visit
- Visits to a specialist more than 30 miles away if there is not a provider close to your home
- Primary care visit
- Prenatal exam
- Postpartum visits between 7 and 84 days after giving birth
- Adult or child SSI visits
- Child lead screening
- A1c screening
- Diabetic eye exam
- Diabetic Kidney Exam
If you need help scheduling one of the above appointments with transportation included, call Member Services at 800-654-9728 (TTY: 711).
Is there a limit on the number of rides I take, or how often I receive transportation?
There are no limits on the number or frequency of rides, as long as they are for medical appointments and meet all qualifications.
Can someone accompany me for rides, such as a caretaker or family member?
Of course. Members are welcome to have someone ride with them. In some cases, children are permitted to accompany you. However, the number of children is limited to seat availability, and members who bring children must have appropriate booster seats.
How do I request transportation service?
Members can call 800-654-9728 to request transportation. Except for same-day urgent care visits, please request transportation at least 48 business hours (not including weekends) before your scheduled appointment to assure coverage for the service. We understand that emergent issues arise and will work actively to fulfill those requests.
Note: Transportation is reviewed on a case-by-case basis and may be subject to Manager or Special Needs approval.
Do I need prior authorization to qualify for transportation services?
No prior authorization from your health care provider is needed. When you call for transportation services, a Priority Partners representative will ask a few questions to see if you qualify for services. Your doctor may also reach out to Priority Partners to request transportation services for you, although no referral is necessary.
Available 24/7
Need More Help?
Our Customer Service team is here to assist you with your application. Contact us to get started:
Mon –Fri, 8am to 5pm EST


